What Is Root Canal Treatment?
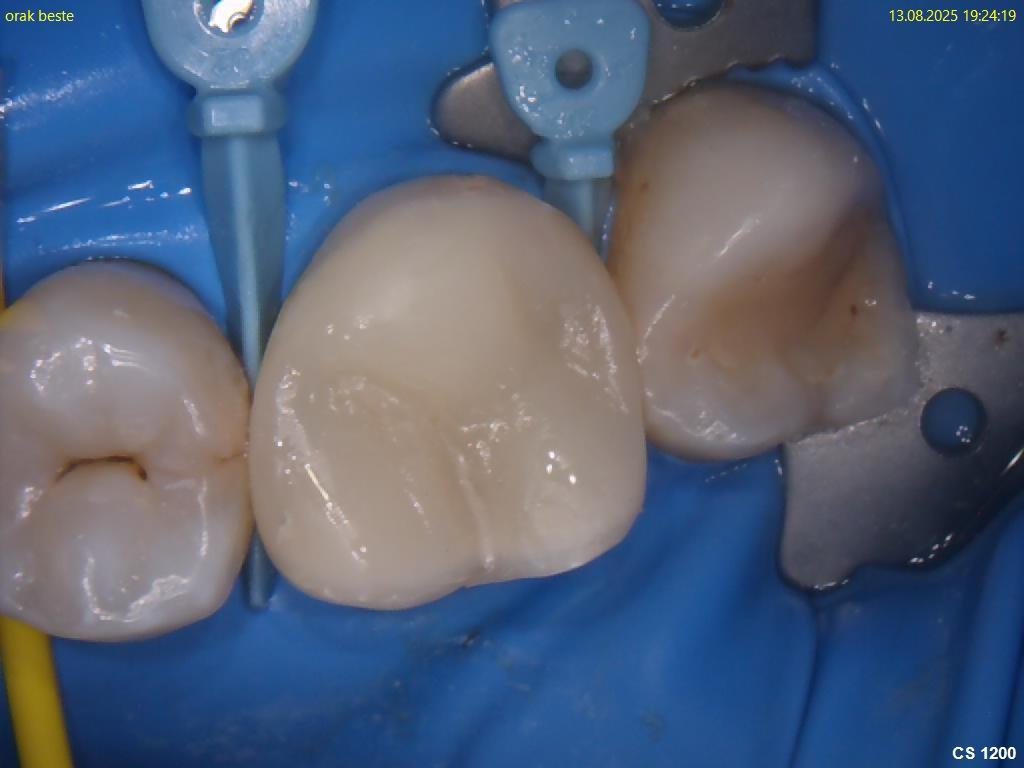
Root canal treatment (endodontic therapy) is a procedure that removes infected, inflamed, or necrotic pulp tissue from the inside of a tooth, cleans and shapes the root canals, and seals them permanently to prevent reinfection. The goal is to save a tooth that would otherwise need to be extracted, preserving its function and preventing the spread of infection to surrounding bone and tissue.
The pulp — the soft tissue inside the tooth containing nerves, blood vessels, and connective tissue — can become infected through untreated deep decay, a crack or fracture, repeated dental procedures on the same tooth, or trauma. When pulp infection spreads into the periapical bone, it can cause a dental abscess, significant pain, and systemic health risk.
Modern root canal treatment at DentARF is performed under magnification using a dental operating microscope, providing up to 25x magnification. This allows our endodontists to identify and treat even the most intricate canal anatomy with precision and confidence. Combined with nickel-titanium rotary instruments, electronic apex locators, and warm vertical condensation of gutta-percha, our protocols are aligned with current best evidence in endodontics.